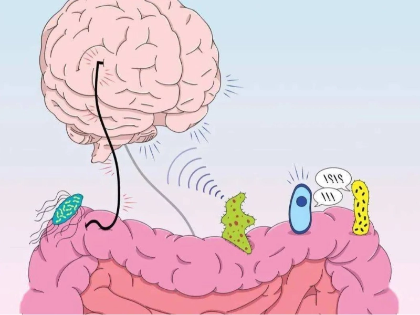
3. The Microbiome’s Influence on Mental Health and Cognitive Function

Recent years have seen a lot of study on the relationship between mental well-being and intestinal health. New research points to a major influence of our gut flora on our mood, cognitive ability, and even mental health susceptibility. A new discipline of research known as “psychobiotics” has emerged from this intriguing relationship between gut flora and brain function.
Studies have revealed that people with some mental health disorders, including anxiety and depression, commonly have changed gut microbiota compositions when compared to healthy people. Although the precise processes are still under research, it is thought that the gut microbiota can affect mental health via several channels including the synthesis of neurotransmitters, control of inflammation, and modification of the stress reaction.
Likewise fascinating is the effect of the gut flora on cognitive ability. Studies have shown that greater cognitive performance—including enhanced memory and attention—is linked to a healthy, varied gut microbiota. On the other hand, disruptions in the gut microbiota have been related to cognitive decline and neurodegenerative diseases including Alzheimer’s disease.
Furthermore included in the idea of the “gut-brain axis” is early brain development. Appropriate brain development and function may depend critically on a healthy gut flora developed in infancy and early childhood. This emphasises how early life gut and brain health is shaped by elements including birth technique, early diet, and antibiotic use.
Recent research have also looked at the possibilities for mental health therapies derived from the microbiome. Some people have found relief from depression and anxiety by means of prebiotics, probiotics, and dietary adjustments supporting a healthy gut flora. Although additional study is required, these results imply that an alternative approach to conventional mental health treatments—nurturing our gut health—may prove useful.
Influence of the gut microbiome on cognitive ability goes beyond mood disorders. Emerging studies point to the microbiome possibly influencing neurodevelopmental problems like autism spectrum disease (ASD). Research on possible microbiome-based treatments has been spurred by several research revealing variations in the gut microbiota makeup between persons with ASD and neurotypical people.
Maintaining a healthy gut microbiome is obviously vital for both our mental and cognitive well-being as we still work to understand the complexity of the gut-brain link. Emphasising the need of including gut health in our whole approach to mental wellbeing, this knowledge provides new options for comprehensive methods to mental health treatment and cognitive enhancement.
4. Nurturing Your Gut Microbiome: Diet and Lifestyle Factors
Given the great influence of the gut microbiome on our general health, it is imperative to know how we could support and preserve a healthy microbial community in our digestive tract. The content and operation of our gut microbiota are much impacted by diet. One of the greatest approaches to support a good gut ecology is a varied, plant-based diet high in fibre.
Prebiotics—that is, foods high in fiber—fruits, vegetables, whole grains, and legumes feed helpful gut flora. These foods give gut bacteria the resources they need to flourish and generate helpful molecules like short-chain fatty acids, which support gut health by anti-inflammatory action.
Still another great complement to a gut-healthy diet are fermented foods. Live helpful bacteria found in foods including yoghurt, kefir, sauerkraut, and kimchi help to vary our gut flora. These meals high in probiotics enhance digestive health and assist to preserve a balanced microbial ecology.
Apart from eating, lifestyle choices also significantly contribute to preserve a good gut flora. Regular exercise has been demonstrated to boost the growth of helpful species and enhance the variety of gut bacteria. Enough sleep is similarly crucial since disturbances in sleep patterns could affect the gut microbiota.
Another absolutely vital component in preserving gut health is stress management. Chronic stress can change the makeup of the gut flora and raise gut permeability, therefore causing inflammation and perhaps other health problems. Deep breathing, yoga, and meditation are among the techniques that support a good gut-brain axis and assist to lower stress.
Meal timing and frequency also affect our gut flora. For example, intermittent fasting has been found to improve gut health by encouraging the growth of helpful bacteria and so strengthening the gut’s natural cleansing mechanisms. Any dietary modification, nevertheless, should be done carefully under the direction of a medical practitioner.
Though sometimes disregarded, hydration is absolutely vital for preserving a healthy intestinal environment. Proper operation of gut bacteria depends on the mucus layer in the intestines, which is maintained in part by enough water intake. Moreover, maintaining good hydration helps general digestive health and can help avoid constipation, therefore affecting the gut flora.
Another crucial component of maintaining your gut microbiome is cutting back on the needless usage of antibiotics. Although treating bacterial illnesses requires antibiotics, abuse of them can upset the delicate equilibrium of gut flora. If antibiotics are required, think about including fermented foods or probiotics to help restore good bacteria.
Our gut flora can also be improved by being in different surroundings and among nature. Studies of those living in more rural locations or those who spend more time outside have revealed more varied gut bacteria. Gardening, hiking, or just spending time in natural surroundings will help one “microbiome rewilding”.