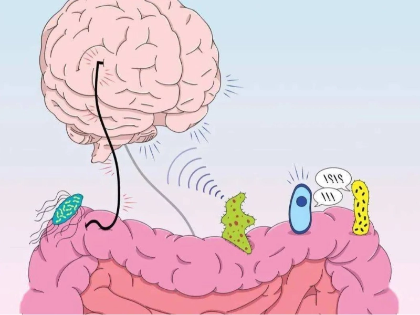
Often referred to as our “second brain,” the gut microbiome is a fascinating realm where trillions of microbes in our digestive tract affect our health, mood, and decision-making. Find the complex link between your stomach and brain, then learn how a better, happier you could result from tending to your microbiome. Discover the most recent studies and useful advice for optimising your gut microbiota.
1. Understanding the Gut Microbiome: A Microscopic Universe Within
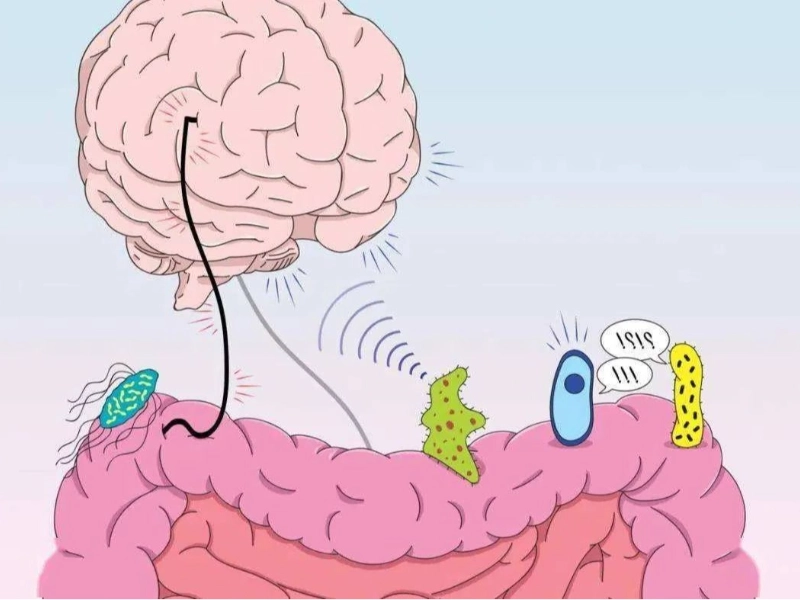
Comprising a large and sophisticated ecology of bacteria, the gut microbiome is found in humans. Trillions of bacteria, viruses, fungus, and other microscopic organisms dwell in this complex community found within our digestive tract. In terms of perspective, by a factor of ten to one the total cells in our body is less than the count of bacteria in our gut. From our immune system to our mental health, this tiny cosmos is absolutely vital for our general well-being.
Beginning at birth, the gut microbiota develops and keeps changing over our lives. Our gut flora is shaped in part by elements including diet, lifestyle, environment, and genes. Like a fingerprint, each person’s microbiome is unique and can be changed by a number of elements. Realising the relevance of the gut microbiome in our life starts with knowing its complexity and variety.
Recent developments in scientific study help to clarify the several purposes of the gut flora. These bacteria help control our immune system, create vital vitamins, and aid in digestion. By vying for resources and space throughout our digestive tract, they also help us ward against dangerous diseases. Beyond just digesting, the gut microbiome affects many facets of our life including our mood, cognitive ability, and even our susceptibility to some diseases.
The general health and operation of the gut microbiota depend critically on its diversity. Generally speaking, a varied microbiome is healthier since it offers a greater spectrum of helpful purposes and is more resistant to perturbations. Diet, age, geography, and drug usage are among the several elements that can affect this variety. A diet high in varied plant-based foods, for example, often encourages a more varied gut microbiome; regular antibiotic usage can lower this diversity.
Realising the dynamic character of the gut microbiota also helps one to understand it. Our gut flora is fast changing in response to several elements, including travel, stress, or dietary changes. This adaptability presents both opportunities and challenges: it implies that, with lifestyle modifications, we can improve our gut health; however, it also means that preserving a healthy microbiome calls constant attention and care.
2. The Gut-Brain Axis: A Two-Way Communication Highway
Scientists sometimes refer to our gut as our “second brain,” since the gut-brain axis—a bidirectional communication system that ties the central nervous system with the enteric nervous system of the gastrointestinal tract—is so strong. Constant information transmission between the gut and the brain made possible by this complex network shapes our ideas, feelings, and general well-being by means of influence.
Operating across several channels, the gut-brain axis is neuronal, endocrine, and immunological system based. One of the longest nerves in the body, the vagus nerve provides direct line of contact between the gut and the brain. This nerve sends signals in both directions, enabling the gut to convey data back to the brain and the brain to control digestive processes.
Crucially in this communication are neurotransmitters, the chemical messengers of the neurological system. Oddly, the gut generates several of these neurotransmitters. For instance, the digestive tract generates almost 90% of the body’s serotonin, a neurotransmitter linked to control of mood. This reality emphasises the important influence our mental state and emotional well-being can have on our gastrointestinal condition.
Other neurotransmitters involved in reward, motivation, and stress response, including dopamine and GABA, also synthesis and control is influenced by the gut flora. This complex interaction between the gut bacteria and neurotransmitter synthesis highlights even more the need of keeping a healthy gut for general mental wellness.
Recent studies have also shown that by the generation of metabolites, the gut microbiota can affect brain activity. Directly influencing brain chemistry, these microbial byproducts can pass the blood-brain barrier Certain gut bacteria, for example, generate short-chain fatty acids, which have neuroprotective properties and could help to lower brain inflammation.
Additionally important for the stress response is the gut-brain axis. Stress can change the makeup of our gut microbiota, which might cause stomach problems. On the other hand, an unbalanced gut flora might alert the brain to produce anxiety or depression signals. This bidirectional link emphasises the need of treating gut health in a whole as well as mental health.